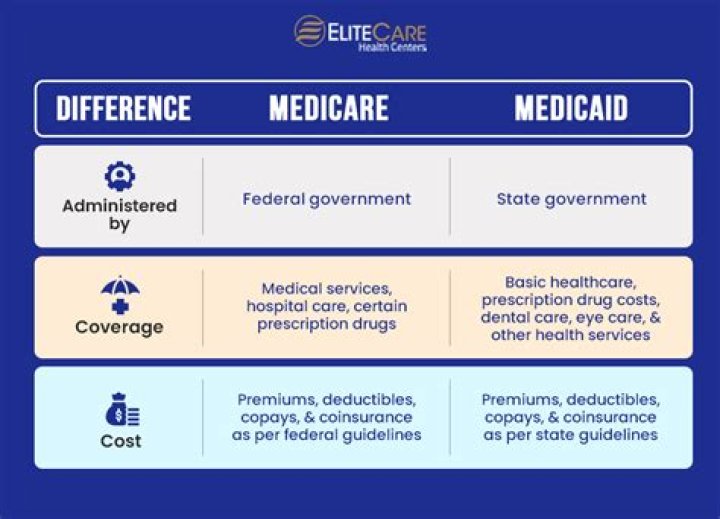
Can my child have Medi-Cal and private insurance?
Yes. Your enrollment in private health coverage will not jeopardize your participation in Medi-Cal. If you have private health coverage and are eligible for Medi-Cal, you may qualify for the Medi-Cal/HIPP program, which can pay for your insurance premiums.
What is the difference between Medi-Cal and Covered California?
Medi-Cal offers low-cost or free health coverage to eligible Californian residents with limited income. Covered California is the state’s health insurance marketplace where Californians can shop for health plans and access financial assistance if they qualify for it.
Who is covered under Medi-Cal?
Many people who are 65 or older or who have disabilities qualify for both Medi-Cal and Medicare. If you qualify for both programs, you will get most of your medical services and prescription drugs through Medicare.
What is considered a household for Medi-Cal?
A household includes the tax filer and any spouse or tax dependents. Your spouse and tax dependents should be included even if they aren’t applying for health insurance.
What is the household income to qualify for Covered California?
According to Covered California income guidelines and salary restrictions, if an individual makes less than $47,520 per year or if a family of four earns wages less than $97,200 per year, then they qualify for government assistance based on their income.
What is notice of action of discontinuance from Medi-Cal?
A Medi-Cal NOA is a written notice that gives Medi-Cal applicants and beneficiaries an explanation of their eligibility for Medi-Cal coverage or benefits. The NOA should include the eligibility decision and effective date of coverage, as well as any changes made in your eligibility status or level of benefits.
What does Noa mean in healthcare?
Notice of Admission
Notice of Admission (NOA)*
How long does Medi-Cal coverage last?
Medi-Cal members must renew their coverage each year to keep their health care benefits. For most members, coverage is renewed automatically….Other Languages keyboard_arrow_up.
| Language | ||
|---|---|---|
| Mandarin | 普通话 | (800) 300-1533 |
| Hmong | Hmoob | (800) 771-2156 |
| Korean | 한국어 | (800) 738-9116 |
| Russian | русский | (800) 778-7695 |
What happens if I don’t report my income change to Medi-Cal?
When you enroll on Covered California, you agree to report any changes, such as an income change, within 30 days. If your income is lower than you thought it would be, you will receive a refund when you file your taxes for any premium assistance that you were eligible for, but did not receive.
What happens if you don’t report income to Medi-Cal?
It carries a potential county jail sentence of one (1) year if charged as a misdemeanor, and a potential county jail sentence of sixteen (16) months, two (2) years or three (3) years if charged as a felony.
How old do you have to be to drop a dependent from your insurance?
Dependent children are eligible to be covered under their parent’s health insurance plan up to age 26. Regarding dropping a dependent from your health insurance coverage, it will depend upon whether you have an individual health insurance policy or whether you are covered under a group health…
Do you have to have maternity coverage if you have dependent child?
However, the preventive-care requirement does not include an exception for dependent children. And although job-based health plans must cover pregnancy-related care for employees and their spouses, federal law doesn’t require the plans to extend maternity coverage to dependent children.
What happens if a pregnant woman does not qualify for Medicaid?
Uninsured pregnant mothers who do not qualify for Medicaid because they make too much money might be eligible for CHIP (Children’s Health Insurance Plan). Some states define an unborn baby as a child and cover the mother’s medical care because the two are entwined.
Can a teenage girl get health insurance if she is pregnant?
Approximately 70% of employer-based group health insurance plans do not cover dependent pregnancies. This means that many teenage and young adult daughters may have to consider alternatives. Two federal laws weigh in on the issue and leave significant gaps.