How do I recoup my Medicare payments?
When Medicare identifies an overpayment, the amount becomes a debt you owe the federal government. Federal law requires we recover all identified overpayments. When you get an overpayment of $25 or more, your MAC initiates overpayment recovery by sending a demand letter requesting repayment.
What is the time period within which provider must report and return a self identified overpayment to insurance?
60 days
The Centers for Medicare & Medicaid Services (CMS) has published a final rule that requires Medicare Parts A and B health care providers and suppliers to report and return overpayments by the later of the date that is 60 days after the date an overpayment was identified, or the due date of any corresponding cost report …
What is Medicare recoupment?
Recoupment Will Occur Automatically by Reduced Medicare Payment for 17 Months. Once recoupment begins, until the amount received under the AAP program is repaid in full, Medicare providers and suppliers will receive reduced Medicare fee-for-service payments.
How many years can Medicare go back?
As of 2021, every state, but California, has a Medicaid Look-Back Period of 60 months (5 years). California has a much more lenient look-back period of 30 months (2.5 years), and New York will be phasing in a 30-month look back for their Community Medicaid beginning April 1, 2021.
Are Medicare accelerated payments taxable?
So as long as the physician group fulfilled its contractual obligation to deliver services, it has a right to keep the payments and therefore the money received for cash basis tax payors is included. It is an acceleration of income into 2020.
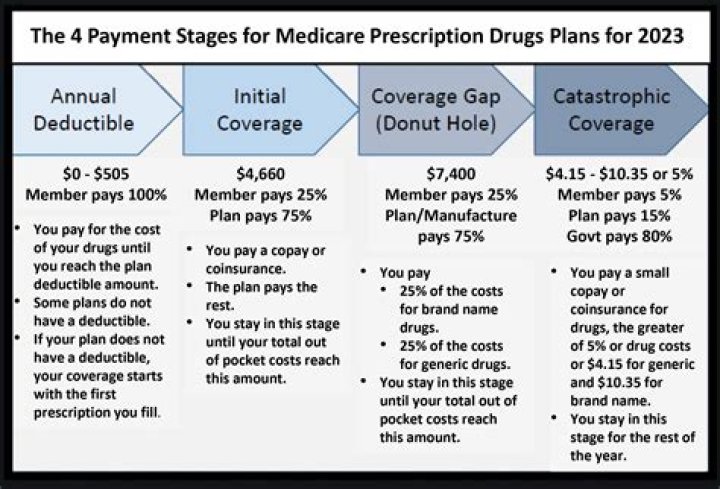
How does recoupment work for Medicare overpayments?
Recoupment may be partial (for example, a percentage of payments recouped) or complete. Upon your request, your MAC can begin recoupment immediately by following the demand letter instructions. Establishing immediate recoupment applies to all current and future debts unless otherwise specified. ● Request Standard Recoupment:
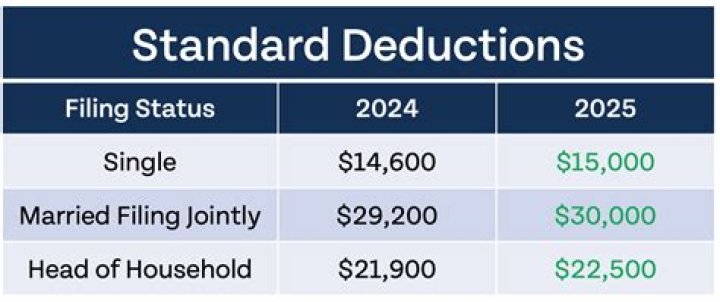
How is the Medicare Part B deductible applied?
The Medicare Part B deductible is applied on a basis of first claim received, first claim applied to the deductible. This means that when the new year starts Medicare will apply your first claim or claims received to your deductible until the full deductible has been satisfied.
What is the limitation on recoupment of provider?
This section implements section 1893 (f) (2) (A) of the Act which limits recoupment of Medicare overpayments if a provider of services or supplier seeks a reconsideration until a decision is rendered by a Qualified Independent Contractor (QIC).
When does Medicare apply the first claim to the deductible?
This means that when the new year starts Medicare will apply your first claim or claims received to your deductible until the full deductible has been satisfied. Keep in mind that the first claim Medicare receives may or may not necessarily be from the first doctor you saw in the New Year.